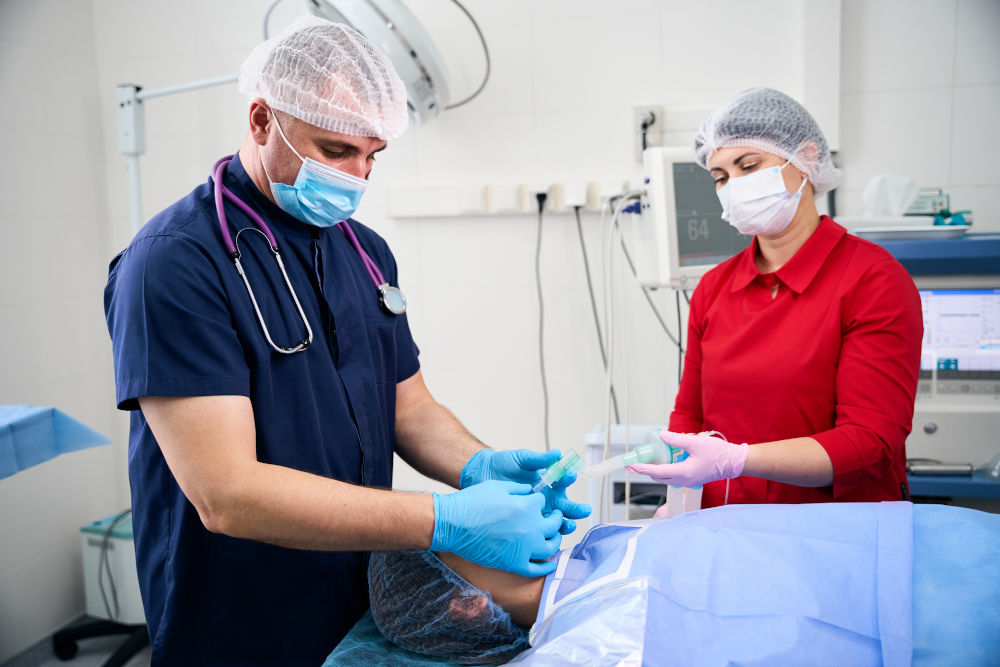
Some patients want to stay aware. Others prefer to “sleep through it.” And somewhere in between lies the real question: what’s actually best for your situation?
When it comes to dental procedures, especially advanced treatments like full-arch restorations, the choice between sedation and general anesthesia isn’t just about comfort. It affects safety, recovery time, cost, and overall experience.
But here’s the catch: many people confuse these two approaches or assume one is simply a “stronger version” of the other. That’s not quite accurate. In reality, sedation and general anesthesia serve different clinical purposes, and choosing the right one depends on a combination of medical, psychological, and procedural factors.
Let’s break it down clearly so you can make a confident, informed decision before your next dental visit.
Key Takeaways
- Sedation dentistry keeps you relaxed and minimally aware, with varying levels from mild drowsiness to deep sedation
- General anesthesia renders you completely unconscious and unaware of the procedure
- Sedation is commonly used for routine or moderately complex treatments, while general anesthesia is reserved for more invasive or medically necessary cases
- The choice depends on medical history, procedure complexity, and patient anxiety levels
- Both methods are safe when administered by trained professionals under proper monitoring
What is the difference between sedation and general anesthesia in dentistry?
At first glance, sedation and general anesthesia may seem interchangeable; they both reduce discomfort and anxiety. But clinically, they serve very different purposes. And if you're considering advanced procedures like full-arch dental implants, this distinction becomes especially important.
Defining sedation in dentistry
Sedation dentistry refers to the use of medications that help patients relax during dental procedures while remaining conscious or semi-conscious. The goal is not to eliminate awareness entirely, but to reduce anxiety, discomfort, and memory of the procedure.
Sedation exists on a spectrum:
- Minimal sedation – You remain fully awake but relaxed
- Moderate sedation (conscious sedation) – You may slur words and not remember much
- Deep sedation – You are on the edge of consciousness, but can still be awakened
Patients often describe sedation as feeling "detached" or "dream-like," rather than asleep.
Defining general anesthesia
General anesthesia, by contrast, is a medically induced state of complete unconsciousness. You are entirely unaware of your surroundings, feel no pain, and have no memory of the procedure.
It involves:
- Suppression of central nervous system activity
- Loss of protective reflexes (such as coughing)
- Requirement for airway support and intensive monitoring
This method is typically reserved for complex surgical procedures, patients with severe dental phobias, or those with special healthcare needs.
Core differences: awareness, purpose, and control
Now, here’s where the distinction becomes clear not just in definition, but in experience and clinical application.
| Feature | Sedation Dentistry | General Anesthesia |
|---|---|---|
| Level of consciousness | Conscious to semi-conscious | Fully unconscious |
| Awareness | Reduced but present | Completely absent |
| Pain perception | Minimal to none | None |
| Memory of procedure | Partial or none | None |
| Airway control | Maintained independently | Often requires support |
| Administered by | Dentist or anesthesiologist (depending on level) | Typically anesthesiologist |
| Recovery time | Shorter | Longer, more intensive |
| Common use cases | Anxiety management, moderate procedures | Surgical interventions, complex cases |
Clinical context and decision-making
- Procedure complexity (e.g., implant surgery vs. routine extraction)
- Patient health status (ASA classification)
- Psychological factors (e.g., dental anxiety or phobia)
- Duration of the procedure
At clinics like All-on-Four Dental Implants Canada, these factors are carefully assessed before recommending an approach. For example, full-mouth restorations may be performed under IV sedation for comfort, or under general anesthesia in specific cases requiring full unconsciousness.
As Dr. Amir Guorgui explains:
“Sedation allows us to keep patients comfortable and cooperative, while still maintaining safety and control. It’s often the ideal balance for implant dentistry.”
Why this distinction matters
Understanding the difference isn’t just academic; it directly impacts:
- Your comfort level during treatment
- The type of monitoring required
- Recovery expectations
- Overall risk profile
And perhaps most importantly, it helps you have a more informed conversation with your dental provider.
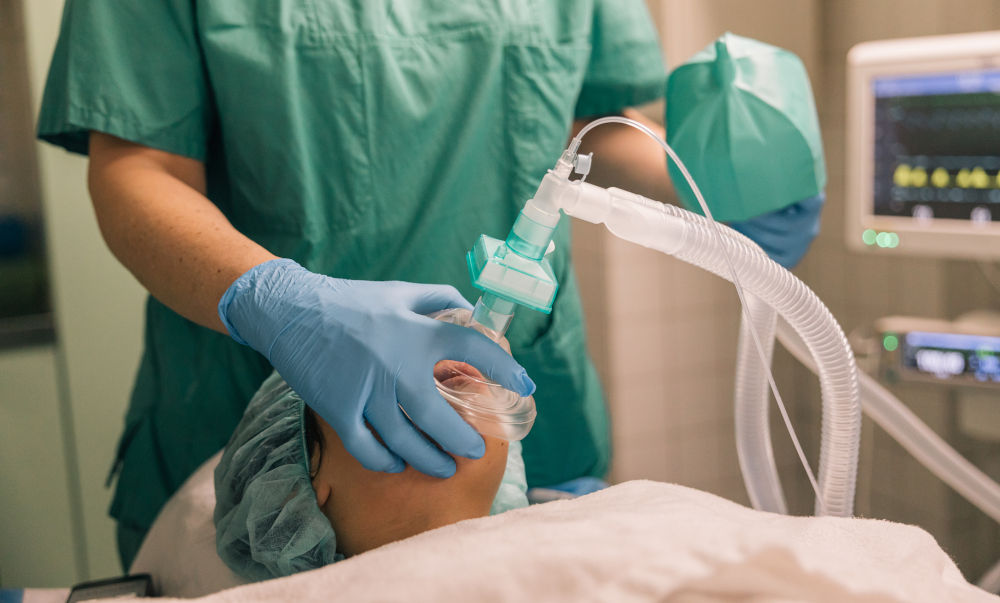
How does sedation work during dental procedures?
It’s easy to think of sedation as simply “being relaxed,” but the reality is far more nuanced. Sedation works by modulating brain activity, specifically targeting the central nervous system to reduce anxiety, perception of pain, and memory formation.
Let’s break it down step by step.
Types of sedation used in dentistry
Different procedures and different patients require different levels of sedation. The most common types include:
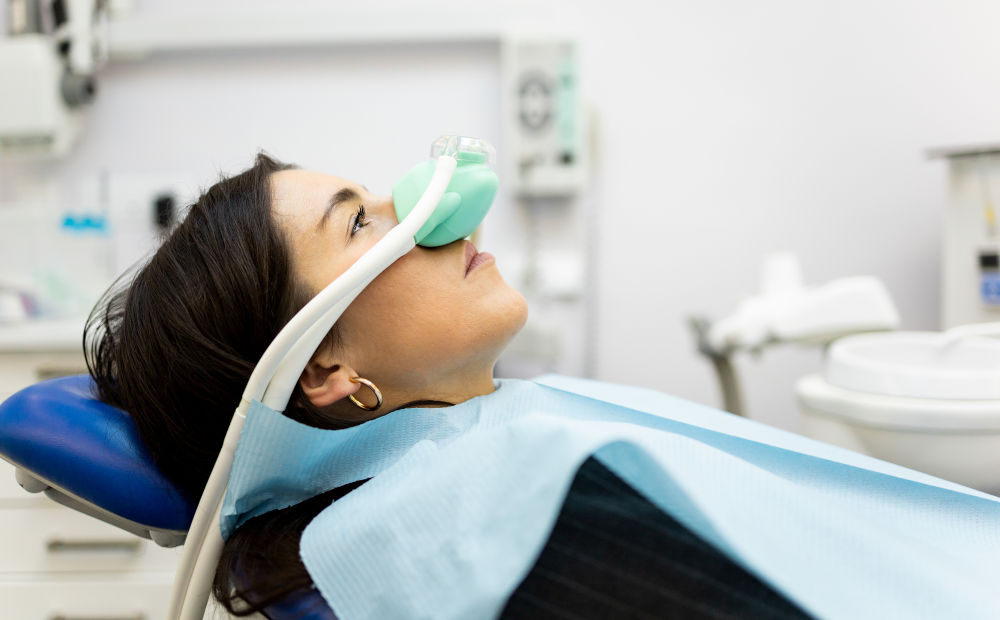
1. Nitrous oxide (laughing gas)
- Inhaled through a mask
- Acts بسرعة (within minutes)
- Produces mild relaxation and euphoria
- Wears off quickly after the mask is removed
This is often used for short, minimally invasive procedures.
2. Oral sedation
- Taken in pill form (e.g., benzodiazepines)
- Produces moderate sedation
- Effects begin within 30–60 minutes
- Patient remains awake but drowsy
Ideal for patients with moderate anxiety.
3. Intravenous (IV) sedation
- Delivered directly into the bloodstream
- Allows precise control of sedation level
- Rapid onset and deeper sedation
- Often used in implant surgery
This is commonly used in advanced procedures, such as those described on the clinic’s implant solutions page.
How sedation affects the brain
Sedative medications, particularly benzodiazepines, enhance the effect of gamma-aminobutyric acid (GABA), a neurotransmitter that inhibits brain activity.
What does that mean in practical terms?
- Reduced neural excitability
- Lower anxiety response
- Decreased awareness of external stimuli
- Impaired memory formation (anterograde amnesia)
Studies in neuropharmacology have shown that this mechanism is responsible for the “calm but awake” state patients experience.
Step-by-step: what the patient experiences
Let’s walk through a typical sedation-assisted dental procedure:
- Pre-assessment
Medical history, medications, and risk factors are reviewed - Administration of sedation
Depending on the type (oral, IV, or inhaled) - Onset phase
Patient begins to feel relaxed, often within minutes (IV/nitrous) or longer (oral) - Procedure begins
Patient remains responsive but calm; time perception may be altered - Monitoring
Vital signs (heart rate, oxygen saturation, blood pressure) are continuously tracked - Recovery phase
Sedation wears off; the patient may feel groggy but typically recovers quickly
What does it feel like?
Patients often report:
- A sense of detachment
- Minimal awareness of sounds or sensations
- Little to no memory afterward
And yet they are still technically conscious.
Evidence-based safety
According to sedation guidelines from dental and anesthesiology associations, sedation is considered safe when:
- Proper patient selection is followed
- Monitoring protocols are adhered to
- Providers are trained in airway management
This is particularly relevant in implant dentistry, where procedures may be longer and more invasive.
What happens during general anesthesia at the dentist?
General anesthesia represents the most controlled and most intensive form of pain and anxiety management in dentistry. It’s not simply “deeper sedation.” It’s a completely different physiological state.
Full unconsciousness: what it really means
Under general anesthesia:
- You are entirely unconscious
- You cannot be awakened by stimulation
- You have no awareness or memory
- Your body does not respond to pain
This state is achieved through a combination of medications that suppress brain activity at multiple levels.
Who administers general anesthesia?
Unlike most sedation techniques, general anesthesia is typically administered by:
- A licensed anesthesiologist or dental anesthesiologist
- In a fully equipped clinical setting
This is because general anesthesia requires:
- Advanced airway management
- Continuous monitoring
- Emergency preparedness
Monitoring and safety protocols
During the procedure, a dedicated professional monitors:
- Oxygen saturation
- Heart rate and rhythm (ECG)
- Blood pressure
- Respiratory function
In many cases, airway support (such as intubation) is required to maintain breathing.
The procedure timeline
Here’s how general anesthesia typically unfolds:
- Pre-operative evaluation
Includes medical clearance and fasting instructions - Induction phase
Medications are administered (IV and/or inhalation) to induce unconsciousness - Maintenance phase
Anesthesia is sustained throughout the procedure - Emergence phase
Medications are reduced, and the patient gradually regains consciousness - Recovery
Patient is monitored in a recovery area until stable
Recovery experience
Unlike sedation, recovery from general anesthesia can involve:
- Grogginess
- Nausea
- Disorientation
- Need for supervision post-procedure
Full recovery may take several hours or longer, depending on the individual.
When is general anesthesia used in dentistry?
It is typically reserved for:
- Extensive surgical procedures
- Patients with severe dental phobia
- Individuals with special needs or an inability to cooperate
- Complex full-mouth reconstructions
Evidence and clinical guidance
Anesthesia literature emphasizes that while general anesthesia is safe, it carries higher risks compared to sedation, including respiratory and cardiovascular complications. That’s why it is used selectively and under strict protocols.
Dr. James C.H. Ko explains:
“General anesthesia provides complete control in complex cases, but it requires a highly trained team and careful planning to ensure patient safety.”
A balanced approach
That decision should always be made in consultation with your dental team, based on:
- Clinical necessity
- Medical history
- Personal comfort level
And sometimes, the best approach is not the most powerful one—but the most appropriate.
What are the main differences between anesthesia and sedation in terms of safety?
Safety is usually the first concern patients raise. And rightly so. While both sedation and general anesthesia are considered safe in modern dentistry, they operate under different risk profiles, monitoring standards, and recovery expectations. The differences are not subtle; they’re foundational.
Understanding risk levels: not equal, but context-dependent
It would be misleading to label one method as simply “safe” and the other as “unsafe.” Instead, safety depends on how well the method matches the clinical situation and patient profile.
Sedation, especially in its minimal to moderate forms, is associated with:
- Lower systemic impact
- Maintenance of protective reflexes (like breathing independently)
- Fewer complications when protocols are followed
General anesthesia, on the other hand, involves:
- Full suppression of consciousness
- Loss of airway control
- Greater reliance on external monitoring and intervention
According to guidance from the Canadian Dental Association and anesthesia safety literature, the deeper the level of sedation, the narrower the margin of safety, which is why general anesthesia requires a more controlled environment.
Side effects and physiological impact
Now, an important point side effects don’t just differ in severity, but in nature.
Sedation side effects may include:
- Drowsiness
- Mild confusion
- Temporary memory loss
- Occasional nausea
These effects are typically short-lived and resolve quickly.
General anesthesia side effects may include:
- Postoperative nausea and vomiting (PONV)
- Sore throat (from airway devices)
- Dizziness and prolonged fatigue
- Rare but serious complications (e.g., respiratory depression)
A review in Anesthesia Progress highlights that while serious complications are rare, they occur more frequently under general anesthesia than conscious sedation, particularly in medically compromised patients.
Recovery time: a practical difference that patients feel immediately
Recovery is where many patients truly notice the distinction.
- Sedation - Often allows same-day recovery with minimal supervision
- General anesthesia - Requires extended monitoring and assistance post-procedure
Patients who undergo sedation, especially nitrous oxide or light IV sedation, can often resume normal activities relatively quickly (though driving restrictions may apply).
With general anesthesia, however:
- You may need several hours in a recovery setting
- A responsible adult must accompany you home
- Full cognitive recovery may take 24 hours or longer
Supervision and clinical requirements
This is where safety protocols become very structured.
| Factor | Sedation | General Anesthesia |
|---|---|---|
| Monitoring level | Basic to advanced (depending on depth) | Advanced, continuous monitoring |
| Airway management | Usually self-maintained | Often requires intervention (e.g., intubation) |
| Personnel required | Dentist + trained staff | Anesthesiologist + surgical team |
| Setting | Dental clinic | Specialized surgical or hospital setting |
| Emergency preparedness | Required | Highly advanced and mandatory |
But here’s the nuance: General anesthesia isn’t inherently unsafe. It’s simply more complex and therefore requires stricter controls.
When is sedation a better option than general anesthesia?
Not every dental procedure and not every patient requires complete unconsciousness. In fact, in many cases, sedation offers a more efficient, cost-effective, and patient-friendly solution.
So, when does sedation clearly come out ahead?
Mild to moderate dental anxiety
Let’s start with one of the most common scenarios: patients who feel anxious, but not overwhelmed.
Sedation is ideal when:
- Anxiety is present but manageable
- The patient can still respond to instructions
- The goal is relaxation, not unconsciousness
This is particularly relevant in procedures like implant placement, where comfort is essential but full anesthesia may not be necessary.
Short to moderately complex procedures
Duration matters. The longer and more invasive a procedure becomes, the more likely general anesthesia may be considered.
But for:
- Single or multiple implant placements
- Tooth extractions
- Periodontal procedures
Sedation often provides sufficient comfort without the added complexity of general anesthesia.
Patient preference and psychological comfort
Some patients don’t want to be “completely out.” And that’s an important consideration.
Sedation allows for:
- A sense of control
- Reduced fear of “losing consciousness.”
- Faster recovery and return to routine
Interestingly, patient satisfaction studies show that many individuals prefer sedation because it balances comfort with awareness.
Cost considerations
General anesthesia typically involves:
- Additional personnel (anesthesiologist)
- Specialized equipment
- Extended recovery resources
This makes it significantly more expensive.
Sedation, especially oral or nitrous oxide, is:
- More accessible
- Less resource-intensive
- Often covered differently by insurance plans
Medical suitability
Certain patients may not be ideal candidates for general anesthesia due to:
- Cardiovascular conditions
- Respiratory issues
- Medication interactions
In these cases, sedation may offer a safer alternative provided it is carefully managed.
Research-backed perspective
Clinical guidelines consistently emphasize that minimal effective intervention is preferred. In other words, if sedation achieves the desired outcome safely, it is often the better choice.
A balanced conclusion
Sedation is not a compromise; it’s often the optimal solution when:
- The procedure is manageable
- The patient is medically stable
- Anxiety can be controlled without full unconsciousness
And in modern implant dentistry, that balance is increasingly the goal.
How do oral sedation and IV sedation compare to general anesthesia?
Not all sedation is created equal. And comparing oral sedation, IV sedation, and general anesthesia reveals a spectrum not just of depth, but of control, predictability, and patient experience.
Oral sedation vs general anesthesia
Oral sedation is often the most accessible entry point into sedation dentistry.
How it works:
- Medication is taken in pill form before the procedure
- Effects develop gradually
- Sedation level is moderate and less adjustable
Key differences from general anesthesia:
- Patient remains conscious
- No airway intervention required
- Lower risk profile
- Less precise control over sedation depth
But here’s the trade-off—oral sedation is less predictable. The same dose can affect patients differently depending on metabolism, weight, and tolerance.
IV sedation vs general anesthesia
IV sedation introduces a new level of precision.
How it works:
- Medication is delivered into the bloodstream
- Onset is rapid (within minutes)
- Sedation level can be adjusted in real time
Compared to general anesthesia:
- Patient is deeply relaxed but not fully unconscious
- Reflexes are usually preserved
- Recovery is faster
- Monitoring is still essential, but less intensive
IV sedation is often considered the closest alternative to general anesthesia without crossing into full unconsciousness.
Step-by-step comparison of patient experience
Let’s break this down from the patient’s perspective:
Oral sedation:
- Take medication before the appointment
- Gradual relaxation
- Drowsy but awake during procedure
- Limited memory afterward
IV sedation:
- IV line placed at the clinic
- Rapid onset of deep relaxation
- Minimal awareness of procedure
- Quick adjustment of sedation level if needed
General anesthesia:
- Induction via IV/inhalation
- Complete unconsciousness
- No awareness or memory
Clarity at a glance
| Feature | Oral Sedation | IV Sedation | General Anesthesia |
|---|---|---|---|
| Consciousness | Awake, drowsy | Semi-conscious | Unconscious |
| Onset time | 30–60 minutes | Minutes | Rapid |
| Control level | Low | High | Very high (by an anesthesiologist) |
| Airway support | Not required | Rarely required | Often required |
| Recovery time | Moderate | Short to moderate | Longer |
| Predictability | Variable | Highly predictable | Highly controlled |
| Typical use | Mild/moderate anxiety | Surgical procedures | Complex surgeries |
Clinical decision-making
Choosing between these options isn’t just about depth; it’s about fit.
Factors include:
- Procedure duration
- Patient anxiety level
- Medical history
- Desired recovery time
Sedation techniques, especially IV sedation, have advanced to the point that they can replace general anesthesia in many cases, offering comparable comfort with fewer risks.
And that’s where modern dentistry is heading: precision, personalization, and minimal necessary intervention.
How long does recovery take for sedation compared to general anesthesia?
Recovery, this is where theory becomes reality. Patients often remember very little about the procedure itself, but they clearly remember how they felt afterward. And the difference between sedation and general anesthesia is particularly noticeable here.
Recovery timelines: what the data shows
Recovery time depends on several factors: the type of medication used, the duration of the procedure, and individual patient characteristics. However, clinical guidelines and anesthesia literature consistently outline clear trends.
Sedation recovery:
- Nitrous oxide - recovery within minutes after discontinuation
- Oral sedation - several hours of drowsiness, with residual effects lasting up to 24 hours
- IV sedation - recovery typically within 1–2 hours, with mild after-effects
General anesthesia recovery:
- Initial recovery (in clinical setting): 1–2 hours or more
- Full cognitive recovery: up to 24–48 hours
- Residual fatigue or nausea may persist beyond that
According to anesthesia recovery studies published in journals such as Anesthesia Progress, patients undergoing general anesthesia consistently require longer observation and delayed return to normal activities compared to those receiving sedation.
Post-operative care: practical differences
The type of care required after the procedure is another major distinction.
After sedation:
- Patients are usually discharged the same day
- A companion is recommended (especially for oral or IV sedation)
- Most normal activities can resume within 24 hours
After general anesthesia:
- Mandatory supervision for at least 24 hours
- Restrictions on driving, decision-making, and physical activity
- Higher likelihood of side effects such as nausea or dizziness
Now, an important nuance while both approaches require caution, general anesthesia imposes stricter limitations on independence during recovery.
Supervision requirements
| Factor | Sedation | General Anesthesia |
|---|---|---|
| Immediate discharge | Yes (most cases) | After extended monitoring |
| Need for an escort | Recommended | Mandatory |
| Home supervision | Optional (case-dependent) | Required (24 hours) |
| Return to normal activity | Within 24 hours | 24–48 hours or longer |
Patient experience: what it actually feels like
Patients recovering from sedation often describe:
- Mild grogginess
- A sense of “waking up quickly.”
- Minimal disruption to daily routine
In contrast, general anesthesia recovery can include:
- Heavier fatigue
- Disorientation upon waking
- Occasional nausea or chills
And here’s the key takeaway: the deeper the level of unconsciousness, the longer and more complex the recovery.
Why recovery time matters clinically
Shorter recovery times are not just convenient, they can reduce:
- Risk of post-operative complications
- Need for extended supervision
- Disruption to daily life
This is one of the reasons sedation is often preferred when clinically appropriate.
Is sedation dentistry safe for all patients?
It’s tempting to think of sedation as universally safe; after all, it’s widely used and generally well-tolerated. But the reality is more nuanced. Sedation is safe when used appropriately, and that means careful patient selection is essential.
Who may not be ideal candidates?
Certain medical conditions can increase the risks associated with sedation:
- Severe respiratory conditions (e.g., COPD, sleep apnea)
- Cardiovascular disease
- Obesity (especially with airway concerns)
- Liver or kidney impairment (affecting drug metabolism)
Patients taking medications that interact with sedatives, such as opioids or certain antidepressants, also require careful evaluation.
Age considerations
Sedation can be safely used across a wide age range, but:
- Children may require specialized dosing and monitoring
- Older adults may have increased sensitivity to sedatives
- Age-related changes in metabolism can prolong drug effects
Guidelines emphasize that dosing must be individualized, not standardized.
Contraindications and precautions
Some situations require additional caution or alternative approaches:
- Pregnancy (especially first trimester)
- History of adverse reactions to sedatives
- Severe anxiety that may paradoxically worsen under mild sedation
Evidence-based safety
Research published in dental anesthesia literature consistently shows that sedation has a strong safety profile when protocols are followed, including:
- Pre-procedure assessment
- Continuous monitoring
- Emergency preparedness
However, complications, though rare, can include respiratory depression or over-sedation.
Dr. Amir Guorgui emphasizes:
“Sedation is very safe, but it’s not one-size-fits-all. A thorough medical evaluation is essential to ensure the best outcome.”
A balanced perspective
Sedation is safe for most patients, but not all. The key lies in:
- Proper screening
- Individualized planning
- Experienced clinical supervision
And when those elements are in place, sedation becomes a highly effective tool in modern dentistry.
How do you choose between sedation and general anesthesia for your treatment?
Choosing between sedation and general anesthesia isn’t just a clinical decision—it’s a collaborative process between patient and provider. And it often starts with a simple question: What level of support does this situation truly require?
Key decision factors
Several variables influence the final recommendation:
1. Anxiety level
- Mild to moderate anxiety - sedation is usually sufficient
- Severe dental phobia - general anesthesia may be considered
2. Procedure complexity
- Short or moderately invasive procedures - sedation
- Extensive surgical interventions - general anesthesia
3. Medical history
- Stable health - wider range of options
- Complex medical conditions - tailored approach
4. Patient preference
Some patients prioritize:
- Faster recovery - sedation
- Complete unconsciousness - general anesthesia
Decision-making at a glance
| Factor | Sedation | General Anesthesia |
|---|---|---|
| Anxiety management | Effective for most patients | Best for extreme cases |
| Procedure type | Moderate complexity | High complexity |
| Recovery time | Shorter | Longer |
| Risk level | Lower | Higher (but controlled) |
| Cost | Lower | Higher |
| Monitoring needs | Moderate | Intensive |
Role of the dental team
This decision is never made in isolation. A qualified dental provider will:
- Review your medical history
- Assess procedural requirements
- Discuss risks and benefits
- Recommend the safest and most effective option
In many modern dental settings, including implant-focused clinics, sedation is often the first-line option, with general anesthesia reserved for specific, well-justified cases.
What are the key takeaways when comparing sedation vs general anesthesia?
After exploring the details, comparisons, and clinical nuances, one thing becomes clear: this is not about choosing the “stronger” option. It’s about choosing the right one.
Summary of core differences
| Category | Sedation | General Anesthesia |
|---|---|---|
| Consciousness | Reduced, but present | Completely absent |
| Safety profile | Lower risk | Higher complexity |
| Recovery time | Short | Longer |
| Monitoring | Moderate | Intensive |
| Cost | More accessible | More expensive |
| Typical use | Anxiety management, moderate procedures | Complex surgical cases |
Clinical insights that matter
- Sedation is often sufficient for most dental procedures, including many implant treatments
- General anesthesia is reserved for specific indications, not routine use
- Recovery and safety considerations often favour sedation when appropriate
Final reflection
So what’s the real takeaway?
- Not every patient needs to be fully unconscious
- Not every procedure requires maximum intervention
- And the best outcomes often come from precision, not intensity
References and further reading
- Canadian Dental Association – Guidelines on sedation and anesthesia
- Anesthesia Progress – Peer-reviewed journal on dental anesthesia
- American Society of Anesthesiologists – Patient safety standards


